First things first, I won’t be one of the 10,000+ attendees in Las Vegas this week at HTLH 2023. Well, at least I won’t be there in person. Thanks to Haley Deming, Beth Kutscher, and the LinkedIn Healthcare Voices Community, I will be there in spirit — keep your eyes peeled. I look forward to the day I can meet in person many of the health tech and digital health people I’ve gotten to know virtually. Who knows, maybe someday I’ll be a speaker and get my own fancy cartoon drawing headshot.
(Note: This post was updated at the end with brief thoughts on General Catalyst’s announcement that it wants to buy a health system.)
There’s been some controversy in recent years about the spectacle of large health tech conferences — HLTH in particular. Some feel the largesse and non-stop party atmosphere clashes with the realities of frontline healthcare challenges and the seriousness of the problems being addressed. Given the difficult funding environment, uncertain macroeconomic conditions, and present struggles of many digital health companies (including some unicorns), there is real risk of coming across as tone deaf. But I’m not here to criticize or serve as a wet blanket. Looking at this year’s agenda, the organizers of HLTH have consciously tried to incorporate the voice of patients and clinicians into this year’s conference. Kudos for that.
For perspective, I’ll be at the Annual Meeting of the American Association of Hip and Knee Surgeons in Dallas next month. Though we don’t have unicorns riding rollercoasters, the meeting features networking, reunions with friends and colleagues, and nightly dinners where many steaks are eaten and adult beverages consumed. Just like HLTH, there are side meetings, meetings within meetings, and meetings outside of meetings. There’s a strong vendor presence and deals will be made. For a few days, around 4600 individuals will take a break from their busy schedules to advance knowledge of hip and knee disorders. (Incidentally, I’ll be speaking at the Business of Arthroplasty Meeting and serving on a symposium panel to discuss the importance of RPM/RTM and virtual care to facilitate the transition to VBC MSK. No fancy headshots unfortunately.) The point is, while you can debate appropriate tone and tenor, large conferences have their place — they play a key role in bringing together people from across the spectrum of an industry. Despite the hype, fluff, and silliness, large meetings can be quite productive. Also, there’s nothing wrong with cutting loose a bit — provided the point of it all doesn’t get lost in all the bacchanalia.
Though I won’t be at HLTH 2023, I have some thoughts about the current state of healthcare technology and innovation that dovetail with many of the topics being covered at the conference. Let’s get into it.
Artificial Intelligence
Artificial intelligence is everywhere. ChatGPT. Bard. LLMs. OpenAI. Stable Diffusion. DallE. The list goes on. It’s not a stretch to say that excitement over AI has singlehandedly propped up the stock market. In fact, as of May, just twenty stocks (most of them AI related) were driving S&P 500 gains. Without them, the index would have been down 1.4%. Along those lines, there is no shortage of excitement for AI in healthcare. In a recent blog post, Dr. Karen DeSalvo (Chief Health Officer of Google) opined that “AI has the potential to transform the health of people on a planetary scale akin to the discovery of penicillin.” That’s a bold statement. Can reality match the hype? I recently put both ChatGPT and Bard to the test and found the results surprising.
Personally, I'm excited about the potential of Generative AI and LLMs to enhance patient engagement and education, make it easier to assimilate medical knowledge, strengthen evidence-based practices, and increase efficiency through ambient documentation and instantaneous medical records summarization. Every clinician dreams of having access to tools that reduce the burden and distraction of time-stealing administrative tasks.
Though Gen AI and LLMs have gotten most of the attention, other forms of AI will be equally impactful (and use cases already exist in healthcare). Predictive AI will allow us to better anticipate problems before they become problems — an ounce of prevention as the saying goes. We're just scratching the surface of the ability to analyze and synthesize data sets to improve outcomes and tailor treatments.
As a Joint Replacement Surgeon, I'm most intrigued by Causal AI and its potential to deliver truly personalized healthcare. We all dream of a world of absolute risk reduction and patient-specific solutions. Using AI/ML to generate cause and effect maps will give us a priori insights into various treatment scenarios at a level not possible in the past.
The mantra for tech companies (big and small) is that AI will not replace doctors. Instead, those who embrace technology will be more favorably positioned for the future than those who resist it. As we stand on the cusp of the AI revolution in healthcare, adherence to this mantra and collaboration between docs and techies will ensure that hype and promise become reality.
“AI has the potential to transform the health of people on a planetary scale akin to the discovery of penicillin.” — Dr. Karen DeSalvo, Chief Health Officer, Google
Healthcare Value
During conversations with health tech and innovation, many are surprised to learn that I’m still in full time clinical practice as an Orthopaedic Surgeon. I see patients on average 2.5 days a week and operate 2.5 days a week. Side gig work in digital health is done after hours, on weekends, and during downtime between surgical procedures. I find advising, investing, and mentoring a key component of achieving work-life harmony and staving off burnout. I also think that straddling the line between frontline clinical practice and healthcare technology/innovation gives me a unique perspective and skillset. In my mind, the key to driving change and evolution in care delivery will be to understand the challenges of real-world medical practice and how best to leverage technology to create innovative models.
I write a lot about what it means to deliver value in healthcare and have experienced VBC in my own practice through CMS’ Bundled Payments for Care Improvement (BPCI) program. Though programs like BPCI and BPCI-A have thus far resulted in mixed results, CMS remains committed to the concept of accountable care. To that end, the recently announced “Make Care Primary” initiative represents the next phase of value-based care. The program is ambitious, and we’ll find out if CMS and CMMI have learned from prior failures. Though much of the focus has been on Alternative Primary Care, MSK is as big an opportunity (if not bigger). The concept of Direct Orthopaedic Care (DOC) is one that I think about a lot.
When it comes to VBC, it’s important to realize that most of the value in healthcare is still delivered on the frontlines -- and it’s not just financial. There is tremendous societal value in replacing an arthritic hip, curing prostate cancer, or preventing a diabetic foot ulcer. Efforts to consumerize, technologize, and virtualize healthcare are destined to fail if their model is to arbitrage or circumvent frontline care and those who deliver it. Few, if any, of these attempts have led to sustainable fixes in part because we continue to devalue (both financially and philosophically) traditional care. Healthcare should continue to evolve, and we can't be dogmatically attached to "the way we've always done things." But it's a mistake to think that frontline healthcare is easily replaceable or that those delivering it are merely interchangeable cogs in the machinery. We aren't perfect, but we're still the primary value creators. As wave after wave of venture capitalists, health system C-suite executives, and payor VPs take the stage at HLTH, let’s hope they don’t lose sight of this fact.
Most of the value in healthcare is still delivered on the frontlines. Let’s hope HLTH attendees and speakers don’t overlook this fact.
Next Generation MSK
Contrary to popular belief, Orthopedic Surgeons (particularly Joint Replacement surgeons) have been on the forefront of the transition to value-based care. The American Association of Hip and Knee Surgeons (AAHKS) worked closely with CMS to provide input on the CJR, BPCI, and BPCI-A programs. Surgeons embraced these programs with an over 50% participation rate (higher than any other medical specialty).
MSK VBC programs have been an unquestionable success in driving cost savings for CMS and improving outcomes. Important lessons have been learned about patient optimization, patient engagement, and care coordination across multi-disciplinary teams. But surgeons dropped out of the programs as CMS and CMMI moved the goal posts, created a race to the bottom, and gradually cut surgeons out of the decision making and care design processes. In short, CMS/CMMI never figured out how to properly reward the work that goes in to successfully implementing these programs (a common criticism of many VBC approaches).
The evolution of VBC MSK care will involve specialists designing and leading novel, condition-specific processes that carefully integrate all aspects of the care spectrum. A flat structure that fosters collaboration between surgeons, physical therapists, behavioral health specialists, primary care providers, case managers, and others is the way. Demonstrable and sustainable value will be a byproduct of such programs and should be rewarded as such.
Don't believe Ortho Surgeons can lead this change? I'm here to prove you wrong. To quote Scott Galloway, “a vision that isn’t widely derided isn’t much of a vision.” However, implementing such a sea change will require collaboration with others trying to innovate in healthcare. The capital and infrastructure necessary to build and implement such programs is beyond the grasp of many specialists. Fragmentation is real. Creating a reproducible and scalable solution, while difficult, is achievable. The best part: you can improve care, reduce costs, engage patients, reward those providing the care, and still have a good business all at the same time.
“A vision that isn’t widely derided isn’t much of a vision.” - Scott Galloway
MSK conditions account for 13% of Medicare beneficiary disease burden (second only to cardiac conditions at 16%). We often hear how employers are being crushed by MSK spend. We know the opportunity; we just need to put it altogether and make it accessible to all. So how do you put it all together in MSK and offer the whole package — value-based care (high quality, high value), improved patient experience, evidence-based and consistent treatment, improved outcomes, reduced costs, increased access? (It's a question I spend a lot of time pondering, and it's why I'm excited about my new role as Medical Director of an ASC Total Joint program.)
I understand and welcome skepticism. After all, what incentive does an Orthopedic Surgeon have to drive value? Fee-for-service is the gift that keeps on giving. The only way to fix MSK is to keep patients away from Orthopods, right? Maybe or maybe not. If ever there was a use case for VBC, it's MSK -- particularly when it comes to the treatment of hip and knee arthritis. Demand is going to outstrip supply. Even with novel payment models, costs of treating arthritis are expected to explode as the population ages (not to mention the alarming rise of joint disease in the 45-55 yo age group). If ever there was a time to figure out how to leverage technology to diagnose, triage, monitor, and support patients with bone, muscle, and joint problems, it's now. If ever there was an opportunity to innovate in healthcare, solve real problems, and reduce costs while rewarding those doing the work, MSK is it.
My vision has always been for a tightly integrated "Arthritis Center of Excellence" that produces value as a byproduct of its philosophy and approach. Condition-specific bundled payments (not those tied to surgical procedures) are the solution to the low value care problem. Smartly implemented technology allows remote monitoring and treatment to make best use of patient and physician time, reduce waste, and improve engagement. Efficient, cost conscious, outpatient centers tied to an ASC can offer transparency, fair pricing, and great outcomes while restoring a sense of autonomy and ownership to the clinicians doing the work. I'm aware that many of these pieces exist in MSK already, it's merely a matter of putting it altogether.
Big Retail in Healthcare
A case study in healthcare FOMO: Big Retailers and alternative primary care.
Recently, news leaked that Walmart is considering a majority purchase of ChenMed, ostensibly to keep pace with Amazon (Iora/One Medical) and CVS (Oak Street Health). The rivalry between Amazon and Walmart is well documented (most recently in Jason Del Rey's excellent book "Winner Sells All"). Having battled it out in online retail, delivery, and grocery (and poached numerous employees from each other), the two companies have turned their focus to healthcare. Add in CVS, and all three companies compete in pharmacy (though CVS has a bit of a leg up as the only one of the three with an insurance arm, Aetna).
The economics of primary care are less favorable than other medical specialties. Health systems purchase PCP groups to control the flow of patients and feed downstream specialist referrals, ancillary services, and hospital-based care (including procedures and surgeries). The value proposition is less clear for Big Retailers who lack many of these verticals. The only real healthcare realted ancillary they have at this point is pharmacy. I'm no pharma expert, but I assume the money being made here is not through selling low-cost generics but through PBMs and specialty drugs (neither of which constitutes VBC). Is feeding into the pharmacy business enough to justify (significant) losses on the primary care side?
All three APCs rely heavily on Medicare Advantage and its risk-based payments, an approach that may be risky given the controversy growing around MA. That ads for MA plans are inescapable these days says a lot about the program. Per KFF, almost half of the Medicare-eligible population is in an MA plan although spending per enrollee is higher in MA than traditional Medicare. Selling MA plans has become a significant driver of growth for insurance companies. But MA headwinds are growing, and the program may not remain as lucrative. CMS has proposed cutting MA rates for 2024 and eliminating many of the risk-based codes it feels were being abused.
Could MA become another CMS VBC program that becomes a race to the bottom? (We in Orthopedics are no strangers to this phenomenon with CJR and BPCI.) If MA reimbursement drops to less favorable or even unsustainable levels, these big bets by Big Retailers may become big flops. These companies could hedge their bets by building additional verticals (much the way health systems do) through bringing specialty care in house and by offering imaging, DME, physical therapy, and other ancillaries. Of course, it's early innings and the rest of us may not be seeing the big picture. Amazon, Walmart, Walgreens, and CVS seem to think they can scale Medicare Advantage profitably. It's not clear if acquisition of VBC primary care clinics is a knee jerk reaction to remain competitive or the first stage of a well thought out plan. The next moves made by these companies will be the most telling.
Not to be forgotten, UHG is playing chess while these three are playing checkers. Its Optum arm has provider groups across the spectrum of healthcare specialties. In 2017, Optum acquired Ambulatory Surgical Center company SCA. Will Amazon or Walmart be bold enough to offer their own insurance product? Does CVS/Aetna have the appetite to enter the Outpatient Surgical Center business? Will Big Retailers figure out how to leverage their control of the patient funnel to make their APC acquisitions worth it? Time will tell. Many C-suite execs at the three companies have staked their careers on these moves, and APCs have benefitted from their FOMO. The amount of turnover in the healthcare leadership at the companies should be cause for concern. The only constant is change.
UHG is playing chess while Big Retailers are playing checkers.
To wrap up, the move that makes the most sense in my mind is for Big Retail to consider MSK as the next entry point. There are more ancillaries here than in any other specialty (PT, imaging, DME, supplements, RPM/RTM, and even ASCs), and the business case is easier to make. MSK has been a huge focal point of VBC, and there will be increasing efforts to tie specialty care to primary care through condition-specific bundles/programs. Curiously, I have a hard time coming up with an acquisition in the MSK space that would make sense for Big Retail or be on the same level as a One Medical, Oak Street, or ChenMed. Most of the focus has been on Virtual PT, and there hasn't been a strong marriage of tech-enabled MSK with brick-and-mortar capabilities.
The traditional MSK market remains fragmented with one exception -- PE-backed MSOs. Would a Big Retailer dare explore acquiring a VBC-focused Ortho platform then tying it to its Alternative Primary Care network? The potential value proposition to employers and CMS in such a model is enormous. Tightly integrating primary care and MSK treatment, though crucially important, has remained elusive. This is a focal point in the recently announced "Making Care Primary" program as referenced previously. (Perhaps this is pure fantasy, but running the MSK arm of such an organization is this bone doc's pipedream!)
Healthcare Consumerism
Is direct-to-consumer healthcare (virtual or otherwise) a sleeping giant or niche that appeals to a limited group of patients?
While many patients are undoubtedly frustrated with the convoluted, expensive, and inaccessible nature of traditional healthcare, selling DTC is not without its challenges. To convince patients to pay out-of-pocket (and occur additional cost on top of their deductibles, co-pays, and premiums), you must deliver a convenient, high-quality experience that justifies the additional expense. In essence, you have to deliver tremendous value.
Many companies have found the DTC bar to be exceedingly high. Acquiring customers can be prohibitively expensive, and it's hard to convince them to keep coming back. A recent article suggested that hospitals and health systems outsource virtual care to a third party — an interesting idea but one that will probably struggle to gain traction. Hospitals and health systems want to control the flow of patients, and telehealth services may not offer a level of differentiation that convinces administrators the risk is worth taking.
Many companies have found the DTC bar to be exceedingly high.
On the other hand, there is certainly a place for a consumer-centric experience. What's appealing about DTC is that it circumvents much of what makes interacting with the traditional healthcare system so frustrating. DTC offers convenient access, transparent pricing, a consumer-focused approach, and the ability to avoid insurance headaches, time-wasting office visits, and the opacity of traditional healthcare. In the end, this is probably what most patients want from healthcare innovation — a better experience.
Can healthcare really be made shoppable?
A Mark Cuban-backed study published recently in JAMA found discrepancies in prices listed on hospital websites and those quoted to "secret shoppers" over the phone. That is, in cases where those prices could be found. Only 63% of top ranked hospitals, 30% of safety net hospitals, and 21% of other facilities provided both listed and verbal price estimates. Of course, there's nothing particularly new or notable here (other than Cuban attaching his name). The lack of transparency, difficulty of finding such information, and wide variation/inconsistencies in pricing are well known issues.
Some of this is certainly intentional obfuscation and flaunting of rules. But much is also a result of the morass created by consolidation. Patchwork health "systems" with increasingly complex administration structures create a disconnect between the C-suite and what's happening on the ground level. The left hand truly doesn't know what the right hand is doing. There's little interest or compunction to change the 30+ year old playbook. Promises of better coordinated, more cost-effective care are rarely realized. Little will change unless there is a credible threat.
There are plenty of efforts underway to make healthcare more transparent, shoppable, and accessible. It remains an uphill battle given the current environment that slaps at the wrists of large incumbents while continually cutting those that could fix the problem off at the knees.
The left hand truly doesn’t know what the right hand is doing. Little will change unless there is a credible threat.
In an ideal world, patients wouldn't have to jump through hoops to get high-quality, cost-effective healthcare (Note: trying to go cheap by diluting the quality of care does not create value). Many patients, when shopping for care, trust word-of-mouth and/or brand reputation. Traditionally, this has meant perceived quality above all else (including price). When thinking about top healthcare brands, quality is what comes to mind first for most — not necessarily experience or cost.
And therein lies an opportunity: develop a healthcare brand that becomes synonymous with cost, quality, and experience. Take the thinking and hoop-jumping out of it. I'm not sure such a thing currently exists in healthcare. We know the top brands that supposedly deliver the best care, but we have no idea if they're competitive on other metrics (often they're significantly more expensive without superior outcomes or patient experience). Healthcare will be fixed when finding high value treatment doesn't require an actuarial degree, SWE-level website sleuthing skills, and a chargemaster interpreter. We don't need billionaire-backed studies to prove it.
Want more consumerism in healthcare? Look no further than Amazon Clinic and its virtual marketplace approach. A la carte pricing is "radical" in healthcare because the system is convoluted and opaque to the point of mass confusion. Many would argue (rightly) that this is intentional and by design. Amazon Clinic, in its current iteration, appears to be an exercise in information gathering regarding patient demand, pricing structure, most effective model of care delivery, etc. It may also be a way for Amazon to determine if they want to move the services in house or establish/acquire their own network of providers.
Amazon Clinic currently functions as a front-end marketplace for patients who have some choice in cost and speed of access. (Less focus on what I think will consistently bring patients back -- quality and experience). Interestingly, digital health companies providing the services (such as SteadyMD and Wheel) function primarily as the backend. They supply a curated network of clinicians while Amazon is responsible for customer acquisition. CAC has been an issue for many virtual care providers and significantly eats into the bottom line. Due to its scale, Amazon may not have the same problem or may be more willing to accept the cost as it tests the model. The company also has more opportunities to use the Clinic as a feeder for other verticals than other virtual care providers (as discussed in the Big Retail section).
Ortho spin: it would seem almost certain that Amazon Clinic is working on a way to add MSK conditions to the platform. There are some challenges -- existing virtual MSK providers may not be well positioned to offer the type of experience Amazon is looking for. Many MSK conditions require longitudinal care, and it can be difficult to parse acute v. chronic problems. Pricing may also be a hang up -- current virtual MSK platforms are built on a value prop of reducing overall MSK spend, not episodes of care.
As a final thought, recent Amazon acquisition One Medical offers its own virtual PT in limited markets called "Motion by One Medical." Scaling this service to Amazon Clinic and across the network of physical One Medial locations provides an interesting opportunity for the hybrid MSK services I'm always going on about.
Digital Health Headwinds
The biggest barrier to adoption and threat to the future of digital health? Reimbursement. No matter how great your idea, how big a problem it solves, or how great an experience it delivers, at some point, somebody must be willing to pay for it.
As discussed previously, D2C is difficult, limits your customer base, and doesn't support health equity. Selling to providers is challenging without a clear ROI (not to mention workflow issues). Overhead costs are rising and reimbursement from traditional care delivery is going down. The appetite for additional costs without additional revenue generation is low. VBC may help alleviate some of these concerns — if it ever becomes widespread. Employers have been a popular target of digital health companies, but there is evidence that they are experiencing solution fatigue and are increasingly wary of fragmentation and lack of evidence.
No matter how great your idea, how big a problem it solves, or how great an experience it delivers, at some point, somebody must be willing to pay for it.
That leaves the government and insurers to take up the cause. CMS has shown some willingness to support digital health solutions with the addition of RPM/RTM codes. Commercial insurers have been less supportive without consensus on what gets covered and by whom.
Defining the value proposition of digital health solutions is still a work in progress. For better or worse, most care is still delivered in a FFS system that depends on CPT codes for reimbursement. This is not an ideal situation for tech solutions that are aimed at making care more efficient, comprehensive, accessible, and patient-friendly. Digital health may never fulfill its potential if sustainable payment mechanisms never materialize. The AMA and greater med tech community believe there is a place for health tech in the future of care delivery -- but do payors?
Of course, it's a two-way street. Digital health companies must prove their ROI both financially and clinically -- not an easy feat. Fragmented point solutions with spurious value propositions supported by flimsy white papers simply aren't going to cut it going forward. But we can't expect to have all the answers right away. It's going to take iteration, patience, and collaboration between health tech companies, CMS, and insurers. Engaging doctors and patients is paramount too. Health tech should support traditional care, not seek to replace it.
Somewhere there's a sweet spot where tech and medicine come together to build something that's worth paying for. I'm not sure we've found that sweet spot yet. It'll be the right blend of old and new and will require re-thinking care delivery in a way that the traditional system may not be quite ready to embrace. Is it worth pursuing? I think so. But little happens sustainably in healthcare without convincing someone to pay for it. And that question remains in doubt.
Health tech should support traditional care, not seek to replace it.
Overheard in many conversations between clinicans and digital health companies: "It gets very complicated very quickly."
It's the conclusion we often reach when I speak with healthcare innovators building patient and clinician facing services. Try as we might, care delivery cannot be completely reduced to virtual, SaaS, or AI/ML solutions. The secret sauce in healthcare has been, and always will be, the human element. This includes both experience and intuition — two things that are hard to completely understand when you come from outside of traditional healthcare.
Which is not to say there isn't a place for building and implementing such solutions. On the contrary, their role has been and will continue to be important. If we're being honest, healthcare has traditionally underutilized technology to the detriment of both doctors and patients. But you cannot replace healthcare soft skills with 1s and 0s.
The key, of course, is to involve those who understand these soft skills early and often in the process. Many meetings and talks at HLTH will end with more questions than answers. That's a good thing. It will spark more conversations on how tools might be better designed to integrate into workflows and surface opportunities to deliver better care with enhanced patient experience.
The most promising digital health companies are those that are willing to re-think their approach based on input from frontline healthcare workers. Neither side is going to be successful by remaining rigid or skeptical of the other. It’s easy to recognize that the human element and years of clinical experience and expertise are the secret sauce to care delivery. Figuring out how to incorporate it into tech solutions gets very complex very quickly.
What metrics determine the success of a digital health platform (or really any healthcare innovation)?
Are improved outcomes and cost reductions the only things that matter? If so, what level of evidence is acceptable -- anecdotal, observational, cohort studies, randomized trials, case-control studies? What if statistical significance doesn't translate to clinical relevance? It's hard enough for solutions to demonstrate improvement in even basic metrics let alone tie those findings to something meaningful. We (rightfully) want companies to start bringing the evidence, but what's the right balance between being letting innovation happen and being skeptical/resistant to change?

In my mind, the solution is to start collecting data early and often and have a plan for how you're going to demonstrate impact. Report preliminary results and detail next steps. As you gain more data and insights, share them. Maybe the hardest part: don't be afraid of negative results and sharing failures/pivots. (Just have a plan to address them). The process is undoubtedly going to be slow and often contra to what the highly competitive startup/innovation environment demands. But the days of inorganic growth and hype as differentiators are (probably) over. You can't stop after a spurious white paper.
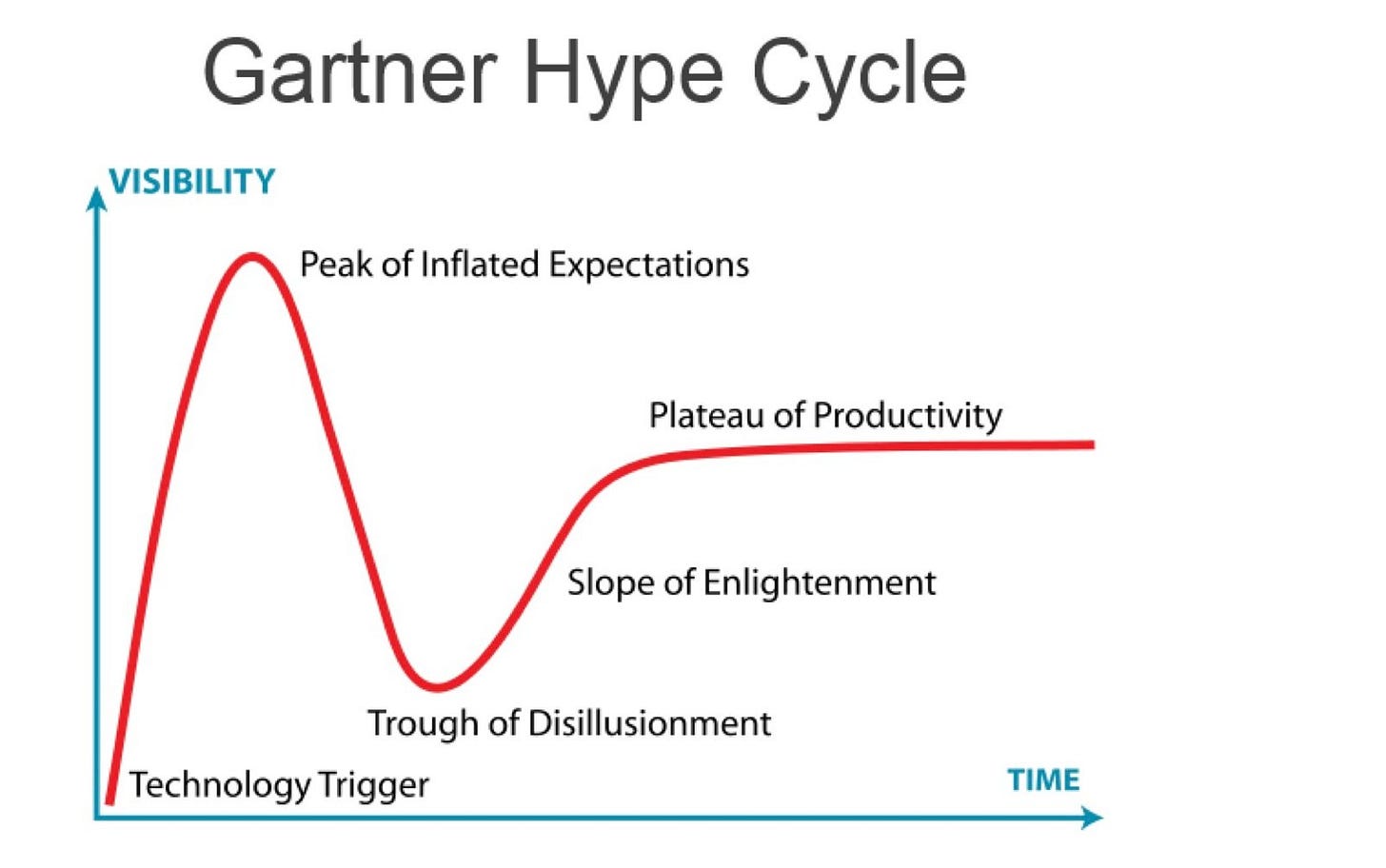
We must also reconcile whether there is value in solely improving patient experience, the tricky business of embracing VBC v. FFS, and clash between what takes precedence: exiting or sustainably fixing problems. These are fundamental issues to address if health tech is to move from the Trough of Disillusionment to the Slope of Enlightenment.
Quick Hitters
In-person and traditional care still matter. Success going forward may depend on engaging health systems and doctors. These are your high value long-term customers.
ROI and clinical impact must be more concrete. It's not enough to propose theoretical savings through avoidance of low value care or move the needle slightly on superficial measurables.
Don't underestimate the importance of the people delivering care. Quality matters. Trust is important. Don't devalue the clinician-patient relationship.
Digital health tools should complement and enhance brick-and-mortar care, not seek to replace it. Integrating into existing workflows and care processes is essential to avoid further fragmentation and siloing.
Health tech still hasn't hit on its strongest use cases. Tech as an innovation in healthcare is a part of the revolution, not the revolution itself.
It's a myth to think that a VBC payment model automatically eliminates perverse incentives or opportunities to game the system. No payment model is unexploitable, and bad actors will be bad actors. CMS should work closely with those providing care to develop programs that realize the goals of VBC — rewarding high value, high quality care that reduces costs and delivers better outcomes.
Value is a byproduct of superior processes and truly innovative models of care delivery. It cannot be carrot and sticked into existence. Creating models that allow entities to succeed by "teaching to the test" (i.e., figuring out how to game the metrics) is not going to drive value.
Some think I'm down on VBC or a VBC skeptic. This couldn't be further from the truth. I just don't think we've seen enough VBC models that make sense, are sustainable, and properly reward what they're meant to reward. CMS has dabbled and iterated but hasn't quite hit on the right formula.
Parting Thoughts
I'm bullish on companies that are building with an eye toward real value through transparency, evidence-based treatment, and integrated, comprehensive care. Alternative primary care clinics being snatched up by Big Retailers have grabbed the headlines (rightly so). Time will tell if they'll be successful (both financially and clinically). But they're not the only ones working toward sustainable VBC. Hopefully healthcare innovation headwinds don’t derail the good work being done.
As exciting as health tech is, we cannot SaaS healthcare into submission or fix the system by trying hard to circumvent it. Yes, there are plenty of opportunities to use software to improve care delivery and valid use cases for virtual, asynchronous, and AI-based tools. And, yes, software is easier to scale, easier to sell, and more likely to attract VC money. There's no reason to fear brick-and-mortar healthcare. While same-y software solutions battle it out on their way to the bottom and struggle to differentiate, more companies are going to recognize the importance of in-person care and sustainability of a hybrid approach.
Sure, it's a more capital-intensive undertaking and longer road to success. But part of what makes great healthcare great healthcare is that you can't easily scale it. Which is not to say you can't build a reproducible model from the ground up, staff it with All-Star people, and deliver an outstanding, high value patient experience. Successful medical practices have been doing this for decades, largely without sophisticated software tools.
Such practices can be successful financially too. Healthcare begs for a Fortune 500 level of efficiency with streamlined administrative processes and a keen eye towards sound business principles. A real healthcare unicorn would be a tech-forward medical practice that runs like a well-oiled machine, frees clinicians to take care of patients, and offers a top-notch patient experience. We tend to underestimate how much patients appreciate face-to-face interactions and overestimate how much care can be delivered through software.
As HTLH 2023 gets underway, I hope the above thoughts spark conversations amongst those attending the meeting. The salad days are over, and there’s much to consider as healthcare technology and innovation enters its next phase. That doesn’t mean the need for novel approaches and thoughtful implementation of technology have ceased to exist. Somewhere amongst the exposition, bloviating, carefully crafted PR messages, VC chest puffing, recycled tropes, gambling, and roller-coaster riding unicorns, I hope there’s room for some real talk about what it’s going to take to make things better.
Bonus Thoughts on HATCo
On Day One of HLTH 2023, General Catalyst made an eye-opening announcement that they tend to buy a health system. I have long contended that, to truly move the needle on healthcare and fully realize the potential of tech and innovation, you’d have to control the entire process. Hospital and health systems are notoriously resistant to chance with long sales cycles and skepticism of anything that threatens the business model. (To be fair, the same could be said of clinicians). Traditional healthcare is reactionary, slow to adopt chance, and fearful of altering the playbook.
Frankly, I thought a Big Tech company or Big Retailer would be the one to make this move. Can a VC firm pull it off? Maybe. GC has deep relationships with existing hospitals and health systems including Jefferson Health, Intermountain, and WellSpan. They have been focusing on “digital transformation” within traditional healthcare for several years now. Running a health system is a different animal. One assumes that they would build a team of healthcare executives who have deep experience running hospitals and healthcare systems. That said, I’m dubious of the ability to change the system by collecting paper champions who have spent their entire careers perpetuating said systems. We’ve seen this approach fail before (Haven). There is no shortage of struggling health systems that may be willing to explore such a sale. There is tremendous potential here to build something great and take a ground up approach to next generation healthcare. There is also tremendous potential to fail spectacularly — with patients and clinicians left to pick up the pieces.